The ovary is the gonadal organ (primary sexual organ) in females. There are two ovaries located within the pelvic cavity, on either side of the uterus. Ovaries contain the developing follicles which produce human egg cells (ova/oocytes) in a cyclic manner, and are also responsible for the secretion of some important hormones such as estrogen and progesterone that maintain the endocrine function related to the reproductive system in females.
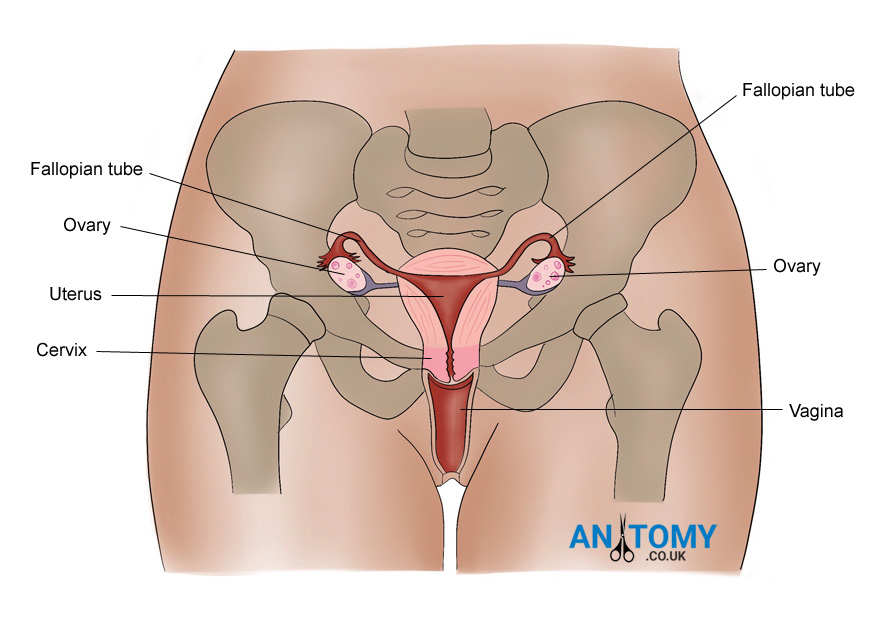
Picture 1: Location of the ovaries in relation to other organs of the female reproductive system
Structure of the Ovary
The ovaries are almond-shaped structures located on either side of the uterus, and closely related to several anatomical structures in the pelvic region. Each ovary has average dimensions of 3 cm (length), 2 cm (breadth), and 1 cm (thickness); hence being smaller than its male analogue – the testis.
The ovaries lie almost vertically in the upright position, and have their upper poles tilted slightly laterally facing the fimbriae at the end of the uterine tubes (fallopian tubes). The lower pole is directed towards the wall of the uterus, and is attached to the uterine wall by the ovarian ligament. The anterior border of the ovary is attached to a double fold of peritoneum extending from the posterior leaf of the broad ligament. This peritoneal extension is called the mesovarium. The rest of the ovarian surface is devoid of peritoneal attachment or lining. The lateral surface of the ovary is attached to the suspensory ligament of the ovary which extends from the wall of the pelvic cavity and carries the blood vessels, lymphatics, and nerves supplying the ovary. Each ovary is said to be located in close relation (laterally) to the ovarian fossa which is a small oval depression in the pelvic wall – marked anteriorly by the external iliac artery, posteriorly by the internal iliac artery and the ureter, and containing the obturator nerve within it.
The ovary is covered by a thick fibrous capsule called tunica albuginea, the outer surface of which is lined by a single layer of cuboidal epithelium which has a misleading name – the germinal epithelium. Inner to the tunica albuginea, the ovarian tissue is divided into two regions; a centrally located medulla and a peripheral cortex. The medulla contains blood vessels, lymphatics and nerves of the ovary. The cortex is made up of ground substance that accommodates a huge number of primordial follicles and the various developing stages of these follicles; primary follicles, secondary follicles, and tertiary (Graafian) follicles. The cortex also contains the remnant tissues following ovulation (cyclic release of ova from the ovaries to the abdominal cavity); the corpus luteum and corpus albicans.

Picture 2: Structure of the Ovary
Blood supply
Ovaries receive their blood supply via ovarian arteries which arise from the abdominal aorta slightly below the level of renal articles (L2 vertebral level). These arteries pass inferolaterally beneath the peritoneum of the posterior abdominal wall, on the psoas major muscle, and cross the pelvic brim and bend medially to traverse through the suspensory ligament and reach the ovary. They also give off a tubular branch to supply the lateral end of the uterine tubes.
The venules of the ovary join together in the medulla and move through the mesovarium and suspensory ligament as a pampiniform plexus which joins to form a pair of veins on either side, and then form a single ovarian vein on either side. The right ovarian vein drains directly to the inferior vena cava, and the left ovarian vein to the left renal vein.
Lymph drainage
Lymphatic vessels follow the venous drainage and drain to the para-aortic nodes situated alongside the aorta close to L2 vertebral level.
Nerve supply
Nerve supply is derived from the T10 spinal segment, via the autonomic nerves of aortic and inferior hypogastric plexuses.

Picture 3: Internal microstructure of the ovary
Development of the Ovary
The ovaries develop from a condensed region in the embryonic gonadal ridge just medial to the mesonephros, in a manner similar to the testes. Primordial germ cells from the embryonic yolk sac move towards the gonadal region and join the developing gonads.
Initially the ovaries are located in the posterior abdominal wall, and they later descend together with their blood and nervous supply. This descent is guided by a condensed mesenchymal tissue named gubernaculum. The ovaries do not descend as far below as the gubernaculum, and are instead arrested inside the pelvis, by the sides of the uterus. The gubernaculum extends further below forming its remnant structures – the round ligament of the uterus and the ovarian ligament – and attaches itself to the labia majora (part of female external genitalia). The mesonephric ducts and tubules usually disappear in females, but their remnants may be found in between the layers of the broad ligament.
Function
The ovary is the primary reproductive organ (gonad) in females, and has two main functions which are (i) Maturation and release of female gametes (ova) in a periodic manner, and (ii) Secretion of female sex hormones (mainly estrogen and progesterone).
Maturation and release of ova (oogenesis)
The ovaries contain about one million primordial follicles (primary oocytes surrounded by epithelium) by the time of birth. Most of these follicles degenerate and only about 40,000 remain at the time of puberty. Small groups of these follicles begin to mature in a cyclic manner under the influence of FSH (Follicular Stimulating Hormone) following puberty. Only one follicle undergoes complete maturation in a given cycle, and the others gradually degenerate. The primordial follicle progressively develops into a primary follicle, a secondary (antral) follicle, and a tertiary (Graafian) follicle. During this development, fluid accumulation and granulosa cell formation occurs around the oocyte. The mature Graafian follicle contains the primary oocyte which divides by meiosis to form the secondary oocyte which is released to the abdominal cavity during ovulation that occurs during the 14th day of the menstrual cycle. The Graafian follicle ruptures, and the released oocyte is held by the fimbriae (finger-like projections) at the end of the uterine tubes. The oocyte is then transported towards the body of the uterus, along the uterine tube, intended for fertilization with a male gamete (sperm). The remnant tissue following the rupture of the Graafian follicle organizes into a yellow colored mass named corpus luteum. The corpus luteum either persists if fertilization and implantation occurs (i.e. pregnancy), or regresses into a fibrous scar named corpus albicans if implantation does not occur within the next 5-10 days.
Secretion of hormones
Estrogen is the primary female sexual hormone, and is synthesized and released mainly by the granulosa cells of developing follicles within the ovaries. This occurs in response to the secretion of FSH following puberty, which stimulates follicle development/maturation. Estrogen has the effect of developing female secondary sexual characteristics after puberty, and causes further development and maturation of female reproductive organs such as the vagina, uterus, and breasts.
Progesterone is secreted mainly by the corpus luteum within the ovaries. This hormone is mainly responsible for preparing the uterus for pregnancy. It also causes development and maturation of female reproductive organs.
Clinical significance
Ovarian cysts
Ovarian cysts are fluid filled cystic spaces found within or on the ovary, usually due to accumulation of fluid around developing follicles. Functional ovarian cysts occur as part of the normal development of follicles, and are usually harmless and regress spontaneously. Pathological ovarian cysts may occur due to an underlying abnormality in the ovary, with most of the cases being benign (non cancerous). Ovarian cysts may cause abdominal or pelvic symptoms only when they are very large or become ruptured; in other instances they are asymptomatic and found incidentally during ultrasound scanning.
Ovarian cancer
Ovarian cancer is one of the most common gynecological cancers. It usually occurs in older women (above 50 years) who have attained menopause. The exact cause is unknown, but the risk of ovarian cancer increases with age, positive family history, being overweight, and presence of other conditions such as endometriosis (presence of parts of uterine inner tissues outside the uterus). It may present with abdominal or pelvic symptoms due to irritation or compression of structures surrounding the ovary.
